Make informed choices that protect your skin from Melanoma.

What is Melanoma?
Melanoma is one of the most serious types of skin cancer, because it can spread beyond the skin more often than many other skin cancers. When discovered early, it can be cured with appropriate treatment1.
Melanin is the pigment in your skin that gives it its colour and helps protect it from the sun’s harmful Ultraviolet rays. Melanin is produced in cells called melanocytes, which are mainly found at the base of the epidermis (the outermost layer of skin). Melanocytes also play a role in determining the colour of your eyes and hair1.
Melanomas occur when melanocytes grow out of control. When skin cells are damaged, new cells may grow out of control and can form a mass of cancerous cells1.
Behind the Shadows: What Causes Melanoma?
The clearest link is between exposure to UV radiation from the sun or tanning devices1.
Exposure to UV radiation causes changes to the DNA (genetic material) of pigment cells and increases the risk of melanoma, especially in people with lighter skin tones. It is important to note that UV radiation does not cause all melanomas. Some melanomas can occur in areas of your body that are not often exposed to sunlight, such as the soles of your feet, palms of your hands and underneath your fingernails or toenails (called acral melanomas)1.
No discrimination: Anyone can get Melanoma
Despite the fact that dark skin does not burn in the sun as easily as fair skin, being in the sun can still damage your skin. Sunlight causes damage through UV rays, therefore even people who don’t burn easily, are still at risk for Melanoma2.
Individuals with darker skin tones tend to have a higher prevalence of advanced-stage melanoma, which correlates with increased mortality3.
The risk of melanoma increases as people age, but melanoma can also develop in younger people. In fact, melanoma is one of the most common cancers in people younger than 30 (especially younger women)4.
DID YOU KNOW?
Melanoma is the 6th most prevalent cancer amongst South African men and the 7th most common cancer amongst women5.
CONTACT YOUR DOCTOR IF YOU NOTICE ANY SIGNS OF MELANOMA.

THERE IS A DARK SIDE TO THE SUN.
IT IS CALLED MELANOMA.
Risk Factors for Melanoma
Common risk factors that make it more likely to develop Melanoma Include1.
Genetic risk factors1
- Lighter skin, hair and eyes
- A tendency to sunburn or have a history of chronic sunburn, especially if you develop redness and blistering
- Many moles (having many or large, unusually shaped moles)
- UV light exposure (extended time exposed to UV radiation from the sun or tanning devices)
- Previous skin cancers
- Childhood cancers
- Weakened or suppressed immune systems (from illnesses or medications that suppresses immune function)
- Family history (about 1 in 10 people with Melanoma have a family history of Melanoma)
- Rare inherited conditions (such as xeroderma pigmentosum, or certain hereditary breast and ovarian syndromes)

Fair skin, freckles and light hair
(as well as blue or green eyes)
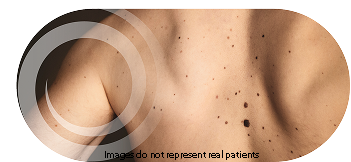
Moles
(having many, irregular, or large moles)
Previous Skin Cancers

Exposure to ultraviolet (UV) rays
from the sun or tanning beds

Weak Immune System

Xerodema Pigmentosum
(a rare inherited condition)

Family History of Melanoma
DID YOU KNOW?
UV radiation is just as dangerous for outdoor labourers and sports people, as well as being on the playground, or when driving to work, as it is when at the beach or pool. Rays can also reflect off surfaces and cause sunburn when it is overcast6.
CONTACT YOUR DOCTOR IF YOU NOTICE ANY SIGNS OF MELANOMA.

THERE IS A DARK SIDE TO THE SUN.
IT IS CALLED MELANOMA.
Signs of Melanoma
Early Detection Can Save Your Life: Know the Signs of Melanoma
Most Melanomas can be seen by the naked eye and can occur anywhere on the skin1,7. However, areas with the most sun exposure, like the trunk, legs, arms and head, are most commonly affected1.
Signs in men with lighter skin colour are more likely be seen on the trunk (chest and back), while in women, they are more likely to start on the legs. The neck and face are other common sites8.
A new spot on the skin – one that changes in size, shape or colour, or one that looks different – is an important warning sign of Melanoma and should be checked by a doctor1.
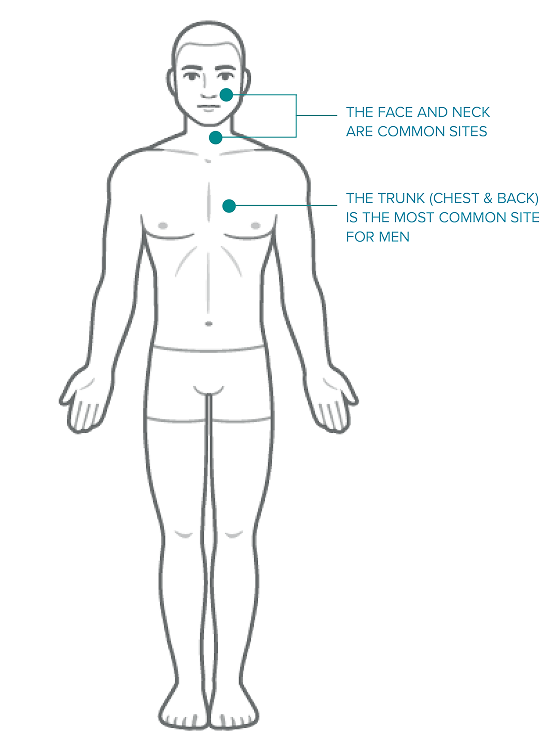
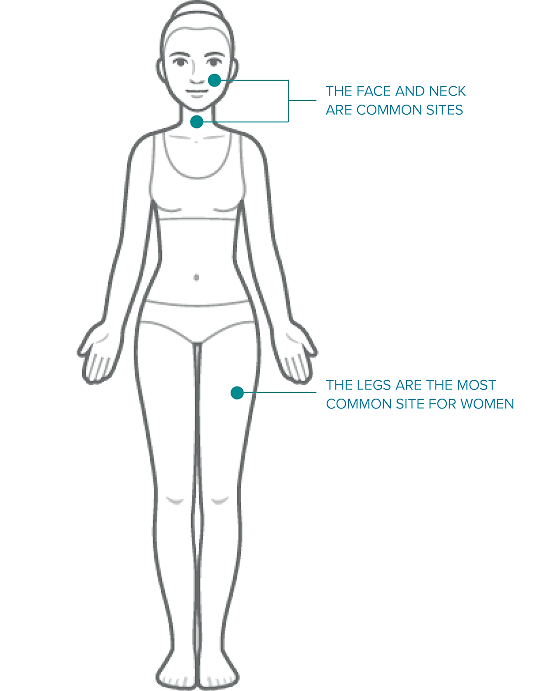
Early Detection of Melanoma

For skin self-exams, following the ABCDE rule can help detect unusual moles and/or signs of Melanoma1

Asymmetry

One half of a mole or spot does not match the other half.

Border

The edges of a spot seem irregular and are difficult to define.

Colour

The colour of the spot is not the same throughout (may be brown, black or sometimes pink, red white or blue).

Diameter
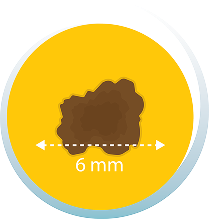
The spot is larger than 6 mm wide (about the size of a pencil eraser).

Evolving

The spot or mole changes its size, shape or colour.
DID YOU KNOW?
EARLY DETECTION MATTERS
Usually, Melanoma grows for a long time under the top layer of skin, but does not grow into the deeper layers of skin. This allows time for skin cancer to be detected early7. When detected in its early stages (before it has spread), Melanoma is easier to treat and cure1,7.
CONTACT YOUR DOCTOR IF YOU NOTICE ANY SIGNS OF MELANOMA.

THERE IS A DARK SIDE TO THE SUN.
IT IS CALLED MELANOMA.
Spot Check
Suspect Melanoma?
ACT | INSIST | ENQUIRE
Have your skin examined by a specialist9.

ACT
A new spot, or a spot that has changed in size, shape, or colour, may be a sign of Melanoma. If you have any of these changes, have your skin checked by a specialist1. Dermatologists can carry out the required tests, to look at a spot more clearly9.
The following basic health tests may be conducted by your doctor1:
- REVIEWING YOUR MEDICAL HISTORY, which is a record of all health issues and treatments you have had in your life, including other cancers.
- A HEAD-TO-TOE SKIN EXAM should include a review of the scalp, face, mouth, hands, feet, torso and extremities, eyes and eyelids, ears, fingers, toes and toenails. This includes examining your skin for lesions.
-
BIOPSY TEST: If you are found to have a lesion of concern on the skin, part or all of it will be removed and sent to a lab to be looked at under a microscope.
This is called a skin biopsy, which is needed to diagnose Melanoma.
In some cases, other tests may be done at the discretion of your doctor1.

INSIST
Insist on a histopathology report for any suspicious moles. This is the only way a diagnosis can be confirmed or ruled out10.
ENQUIRE
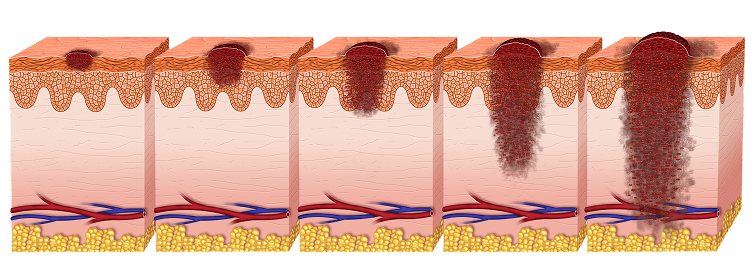
Understanding the melanoma stage is very important, as it is needed to make appropriate treatment decisions. Staging helps describe the depth of the melanoma, whether any lymph nodes are involved, and whether or not the melanoma has spread (metastasized)1.

DID YOU KNOW?
Knowing your own skin is important for early detection. Show your doctor any changes or differences where your skin might look abnormal or different to you1.
CONTACT YOUR DOCTOR IF YOU NOTICE ANY SIGNS OF MELANOMA.

THERE IS A DARK SIDE TO THE SUN.
IT IS CALLED MELANOMA.
Treatment of Melanoma
There are different types of treatment available for people with Melanoma. There are several factors that a doctor will use, to decide on which treatment to use11.
During treatment, follow-up tests or check-ups will need to be carried out. Some of the tests that were done to diagnose or stage the cancer will be repeated, to see how well the treatment is working11.
Decisions about whether to continue, change, or stop treatment, may be based on the results of these tests. Some of the tests will continue to be done from time, to time after treatment has ended. The results of these tests can show if the condition has changed, or if the cancer has recurred11.
Treatment options for Melanoma include1:
- Surgery
- Radiation therapy
- Immunotherapy
- Chemotherapy
- Targeted therapy
Talk to your doctor about your treatment plan and what it means for your stage of Melanoma.
DID YOU KNOW?
EARLY DETECTION CAN SAVE LIVES
Melanoma is most likely curable when detected early1.
CONTACT YOUR DOCTOR IF YOU NOTICE ANY SIGNS OF MELANOMA.

THERE IS A DARK SIDE TO THE SUN.
IT IS CALLED MELANOMA.
Protection
Ways to lower your risk for Melanoma
Limit your exposure to UV rays
Seek shade, especially between 10am and 4pm. Simply staying in the shade is one of the best ways to limit your UV exposure6,12. If you need to be outside during these hours, seek shade under a tree or an umbrella6.
Slip! Slop! Slap! and Wrap!12

Slip on a shirt:
Cover up with protective clothing and swimsuits6.

Slop on sunscreen
- Use a sunscreen with an SPF of between 20 & 30, and 50 for fair to very fair skin6.
- Don’t use a product that has been opened and used after a year has passed or if it has expired6.
- Apply sunscreen 20 minutes before you go outside and reapply at least every 2 hours, after towel drying, perspiring or swimming6.

Slap on a hat:
Wear thickly-woven fabric hats with wide brims – avoid caps where the neck and ears are exposed6.

Wrap on sunglasses
Wear sunglasses with a UV protection rating of UV400, to protect the eyes and sensitive skin around them6,12.

Avoid using tanning beds and sunlamps
Tanning lamps give off UV rays that can cause long-term skin damage and have been linked to an increased risk of Melanoma, especially if started before a person is 30 years old1,12. Most dermatologists (skin doctors) and health organisations do not recommend the use of tanning beds and sunlamps12.

Do a monthly spot check
Check your skin carefully every month. Ask a family member or friend to help examine your back and the top of your head. Remember the ABCDE rule – if you are concerned about a particular spot, see a doctor or Dermatologist immediately6.
Be Proactive
Against Melanoma12
CHECK YOUR SKIN REGULARLY.
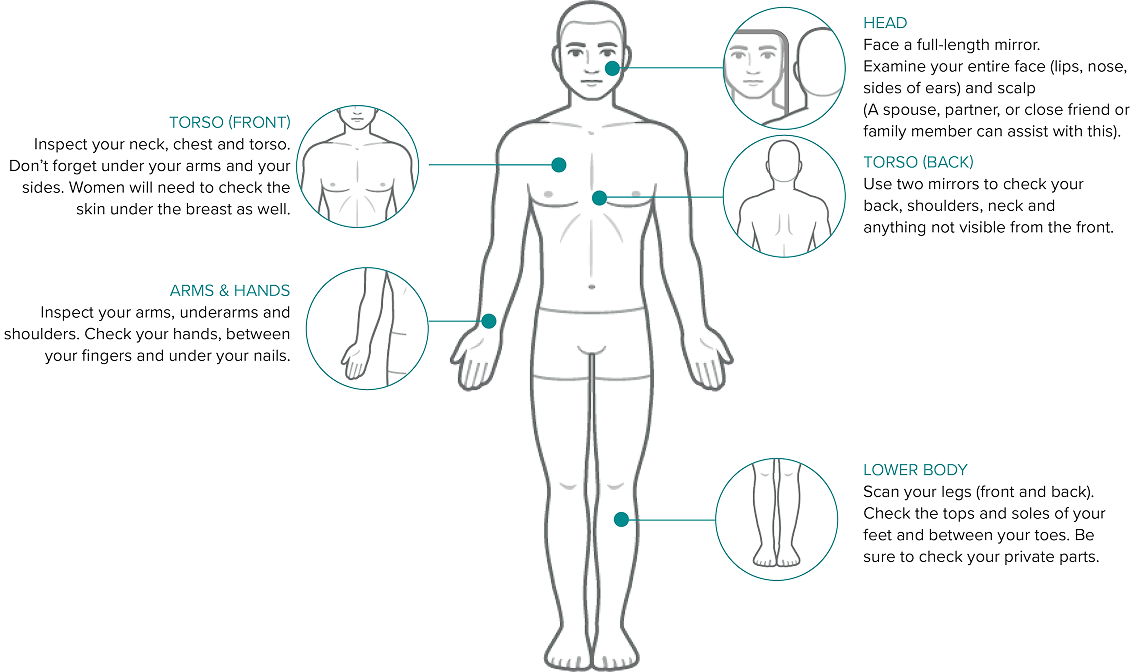
Skin Self-Exam
Skin self-exam – what you will need13:
- A well-lit room
- A full-length mirror
- A hand-held mirror, to look at areas that are hard to see
- A spouse, partner, or close friend or family member, to help you with hard-to-see areas like your back or scalp
References
-
National Comprehensive Cancer Network (NCCN). Guidelines for patients. Melanoma. 2025.
Available from: https://www.nccn.org/patients/guidelines/content/PDF/melanoma-patient.pdf. Accessed 25 June 2025. -
National Cancer Institute (NCI). Skin Cancer in People with Darker Skin. 12 November 2024.
Available from: https://www.cancer.gov/types/skin/skin-cancer-in-black-or-brown-skin. Accessed 25 June 2025. -
Thompson B, Jenkins T, Sánchez JP, et al. Melanoma: Does It Present Differently in Darker Skin Tones? MedEdPORTAL. 2023 May 9;19:11311.
Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC10166772/. Accessed 25 June 2025. -
American Cancer Society. Risk Factors for Melanoma Skin Cancer. 27 October 2023.
Available from:https://www.cancer.org/cancer/types/melanoma-skin-cancer/causes-risks-prevention/risk-factors.html. Accessed 25 June 2025. . -
The Cancer Association of South Africa (CANSA). Melanoma. C2025.
Available from: https://cansa.org.za/melanoma/. Accessed 25 June 2025. -
The Cancer Association of South Africa. Be SunSmart Everywhere. 10 December 2024.
Available from: https://cansa.org.za/be-sunsmart/. Accessed 25 June 2025. -
National Cancer Institute (NCI). Cancer Screening (PDQ®) – Patient Version. 15 may 2025.
Available from: https://www.cancer.gov/types/skin/patient/skin-screening-pdq. Accessed 25 June 2025. -
American Cancer Society. About Melanoma Skin Cancer. 21 February 2024.
Available from: https://www.cancer.org/content/dam/CRC/PDF/Public/8823.00.pdf. Accessed 25 June 2025. -
American Cancer Society. Can Melanoma skin cancer be found early? 27 October 2023.
Available from: https://www.cancer.org/cancer/types/melanoma-skin-cancer/detection-diagnosis-staging/detection.html. Accessed 25 June 2025. - Puckett Y, Wilson AM, Farci F, et al. Melanoma Pathology. [Updated 2024 Jul 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459367/. Accessed 25 June 2025
-
National Cancer Institute (NCI). Melanoma Treatment (PDQ®) – Patient Version. 16 May 2024.
Available from: https://www.cancer.gov/types/skin/patient/melanoma-treatment-pdq. Accessed 25 June 2025. -
American Cancer Society. Can Melanoma Skin Cancer Be Prevented? 27 October 2023.
Available from: https://www.cancer.org/cancer/types/melanoma-skin-cancer/causes-risks-prevention/prevention.html. Accessed 25 June 2025. -
American Cancer Society. How to do a skin self-exam. 26 June 2024.
Available from: https://www.cancer.org/cancer/risk-prevention/sun-and-uv/skin-exams.html. Accessed 25 June 2025.
ZA-NON-01013. Exp: 06/2027